Is your IBS embarrassing? New research reveals the overwhelming effect of the chronic condition on people’s lives, with 45 per cent of people with it reporting feeling depressed. Leading gastroenterologist Dr Simon Smale reveals the seven ways to beat your IBS for good
Almost one in five people suffer with IBS in the UK, and unfortunately the chronic condition doesn’t just effect the gut. Bloating, diarrhoea and stomach aches, common symptoms of IBS, are causing love lives, sleep, confidence and social lives to suffer, too, a new survey has revealed. ‘Living with IBS in the UK’, surveyed 1000 adults with IBS and highlighted how the illness is impacting quality of lives. It’s no wonder, then, that a disheartening 46 per cent of respondents said their IBS is making them feel depressed.
72 per cent report that stress is a major cause of their flare-ups
With IBS comes a social stigma, with 38 per cent of respondents saying their IBS is a huge embarrassment to them, leading to social isolation. What should be a fun girls’ night out can become an onset of anxiety for IBS sufferers, with over half being terrified they won’t be able to access a bathroom in time despite mapping the nearest toilets before heading out.
Even around close friends and family, 70 per cent of respondents are suffering in silence, according to the study. The embarrassment of the illness is extending to romantic relationships too; 32 per cent have not told their partner about their daily struggle, or have even sacrificed their relationship entirely.

IBS is not only impacting peoples work and social life. Getting a good night sleep is a task, with 35 per cent of people struggling to get a sleeping pattern. This can exacerbate stress, which 72 per cent of people said is a major cause of IBS itself.
IBS is a complex and unpredictable condition. Healthista spoke to leading expert Dr Simon Smale about how to manage IBS, and therefore its hold on people’s lives.
MORE: 7 myths about IBS even smart women believe
1. Diet
Following NICE guidelines, the first thing Simon recommends is diet manipulation. What we put into our gut significantly effects the way our gut behaves, and certain things can exacerbate IBS symptoms. ‘People need to eat regularly, never leaving large amounts of time between meals’, says Simon. ‘It’s also not a good idea to eat all your calories in one go at the end of the day. Some of my patients will wait till the end of the day to eat a takeaway with a beer, which is not a good idea’.
Diet fizzy contain a carbohydrate that is difficult to digest
Caffeine should be kept to three drinks a day, and nicotine, alcohol and fizzy drinks should be avoided. However, diet fizzy drinks also contain a carbohydrate that is difficult to digest. Spicy food often contains a chemical called capsaicin which can trigger receptors (TRPV1 receptors) in the gut. These influence sensation and hence motility within the gut, which may be why extremely spicy food can trigger diarrhoea in susceptible individuals. These are common flare-up triggers, however all patients will vary.

Simon also draws upon FODMAP, an acronym for fermentable oligosaccharides, disaccharides, monosaccharides, and polyols. ‘These are complex sugars, or short chain carbohydrates, which we as human beings don’t have the proteins to digest, but the bacteria that live in our gut do’, explains Simon. ‘When they get the bit of the bowel called the colon, they can ferment and cause bloating and diarrhoea’. This can be said the same for wheat and grains, which are commonly chosen to be avoided by IBS patients. ‘Avoiding those foods that contain those sugars can potentially make symptoms better, but it should be done with the support of a trained professional such as a dietician’, says Simon.
With long waiting lists on the NHS, a number of phone apps can help with tracking diet. ‘I would recommend The Monash University Low FODMAP diet app developed by experts at Monash University and the FODMAP by FM app, developed by Kings College Hospital’.
MORE: Is this the diet to end IBS?
2. Exercise
‘There are a number of studies that suggest exercise is beneficial for those with IBS’, Simon reveals. ‘20-60 mins to moderate to vigorous exercise three to five times a week, depending on your ability, is likely to have a positive effect on your gut motility and bowel function.’
Results from a small study on 102 patients of IBS, published in the NCBI, suggests the same. Patients were randomly assigned to a physical activity group (12 weeks of moderate to vigorous exercise – 20-60 minutes three times a week) or a control group (maintaining their same lifestyle). Although 27 did not complete the study, of those who did, researchers found patients who had the most significant change in fitness had a significant improvement in their overall IBS by rating their severity.
Simon recognises a significant number of people avoid doing exercise because they are worried about their bowels, therefore recommend to plan it at times of the day your bowels are more settled. ‘Gently increase your amount of exercise, something you enjoy even if it is just walking the dog, as there is no doubt long term benefits to the health of your gut’, he says.
3. Managing stress
72 per cent of people with IBS recognise stress as a trigger of an IBS flare up, according to the Living with IBS in the UK survey. ‘But avoiding stress is very difficult and of course most of us tend to try and get on with life’, says Simon. ‘About a third of people have their social life (37 per cent) or sleep (34 per cent) effected by IBS, and that can only add to the stress’.

‘In some people there is a vicious circle, but there is a complex interaction between stress, diet, sleep and everything else in people’s lives. Whilst stress can cause an exacerbation with IBS, one of the problems of that exacerbation is you can get stressed about your bowels, perpetuating the symptoms’.
When you’re sleep deprived a hormone called ghrelin drives your appetite
Taking time every day to relax as well as a consistent and deep sleep pattern is a first step to reducing stress. Those who sleep less often make poorer food choices due to biological factors. ‘When you’re sleep deprived a hormone called ghrelin drives your appetite and food choices towards foods that are high in calories and of greater value in terms of energy – sugary and fatty’, Simon clarifies.
There are a range of phone apps that can help with sleep (such as Sleepio) and meditation (Headspace). ‘Even seeking help of a counsellor or physiologist can be transformative’, advises Simon.
MORE: 6 best apps for mental health
4. Probiotics
We have more bacterial DNA inside our bodies than human DNA, and where we thought the bugs living inside us had no relevance to our diseases 20 years ago, Simon says they are becomingly exceedingly relevant. Not only IBS, but mental illnesses and obesity, for example. ‘It’s clear that there are bacteria in our gut that can promote inflammation or dampen it down’, says Simon. ‘There are also bacteria that can affect the chemistry in our brains and the nerves and therefore the sensitivity in our gut. As a result, it’s not surprising that manipulating gut bacteria can affect the way our IBS behaves.’
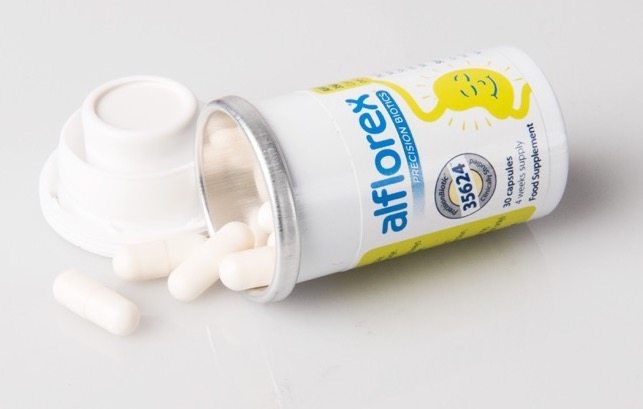
How do you make sure a probiotic ticks the boxes? ‘There are a number of companies now marketing probiotics, including Alflorex, which provide good scientific studies’, says Simon. Alflorex contains the natural live culture, 35624, which has been shown in clinical trials to reduce symptoms such as abdominal pain, unpredictable bowel movements and bloating.
MORE: A cure for IBS? This probiotic pill is scientifically proven to help
5. Over the counter drugs
Drugs, mostly available over the counter, can be split into three different categories. The first are those which effect the sensitivity of the bowel, such as peppermint oil, which work on the same receptors as the capsicum, the chemical found in peppers that can worsen symptoms. Secondly, there are drugs that effect motility of the bowels. These can either slow the system down, which is good for diarrhoea, or speed the system up, good for constipation and softening stool. ‘People need to be cautious that they don’t flip between diarrhoea and constipation with the use of drugs’, says Simon.
Lastly, there are drugs which effect the nervous processing of the gut – drugs like amitriptyline. Despite options being accessible in the chemist, Simon is impartial to their benefits. ‘The best of these dugs works with one in six people, and there is a big placebo response. Most people won’t need to take drugs for their IBS if they can manage their lifestyle’, he says.
6. Intolerance testing
The role of intolerance testing in IBS management, such as the YorkTest, is scientifically debated. Any testing should be done with careful clinical assessment of the patient being integral to the interpretation of the test.
Firstly, Simon notes the importance of knowing the difference between allergies and intolerances. Food allergies are immunological responses to one particular food, which produce inflammation, rash or swelling, for example. A food intolerance does not involve the immune system responding, in the sense of causing inflammation and the symptoms are often limited to the gut, for example bloating and diarrhoea.
Food intolerances can play a part in producing irritable bowel symptoms, but not every person with IBS will have food intolerances, and not every person with a food intolerance will have IBS. Tests are available, such as the York test, skin test, or blood tests. They can involve as little as a finger prick blood test to screen for antibody reactions to foods.
MORE: Is lactose intolerance a myth?
The risk is you exclude something from your diet you really need
‘Currently, I wouldn’t recommend going for an intolerance test. But that doesn’t mean that I don’t have patients that have done intolerance testing, changed their diet because of it, and got better. The trouble is, I know changing people’s diets can radically change their symptoms’, he says. ‘The risk is not necessarily that you exclude things from the diet, but that you are excluding something you need in your diet. You need to do it in a structured way whereby A. you can reintroduce things into your diet, and B. your diet still includes all your vital vitamins and nutrients.’
7. Hypnotherapy
Although there is a small amount of trials to support the theory, Simon notes hypnotherapy as undoubtedly beneficial for a number of those with IBS. This is because the brain and bowel are connected – hence why we all may get butterflies or an upset stomach when we are nervous. ‘When you look at the brain and gut as being a dynamic thing that all of us have, what IBS is, in a way, is a disorder of this complex interaction between brain and gut and what we put in the tank’, says Simon.
The brain and bowel are connected. IBS is a disorder of this complex interaction
Researchers at Withington Hospital, where the first UK hypnotherapy unit was established, concluded that hypnotherapy was a viable therapeutic option for treating IBS. They monitored 200 patients after undergoing one hour gut-directed therapy for 12 weeks, and found 70 per cent of patients responded well. What’s more, when the participants were questioned five years later, the improvement had hardly deteriorated.
Simon admits science does not yet understand the complex connection between the gut and brain, which was only discovered 20 or so years ago. He advises first improving diet and lifestyle, taking caution with intolerance tests and exclusion diets, and moving to further options if symptoms persist.
Dr Simon Smale is a consultant gastroenterologist providing outpatient, in-patient and endoscopy services both privately at the York Nuffield Hospital and also for the NHS at York Hospital NHS Foundation Trust.
Reader offer
We’re excited to offer an exclusive 10% discount for Healthista readers for Alflorex adult capsules. Simply use the discount code HEALTHISTA at checkout, valid until 31st May 2017.
DISCLAIMER: We aim to ensure that the contents of this article (materials) are accurate and consistent with current knowledge and practice. However, the materials are not exhaustive, presenting some but not all aspects of conditions and cannot always reflect all the most recent medical research in all areas. We make no guarantees, representations or warranties whether express or implied that the materials are accurate, complete or up-to-date.
Accordingly the materials are presented for information purposes only and are not intended to amount to advice on which reliance should be placed. The materials in no way replace the professional medical advice or treatment of a doctor or other qualified practitioner and cannot and should not be used as a basis for diagnosis or choice of treatment. If you have health problems you should consult a doctor for a full and proper diagnosis based on an analysis of any symptoms and your medical history.
READ MORE
How I overcame the IBS that’s plagued me since I was 8
Probiotics – 13 things you REALLY need to know
10-minute yoga for anxiety to let all that tension go
Like this article? Sign up to our newsletter to get more articles like this delivered straight to your inbox.