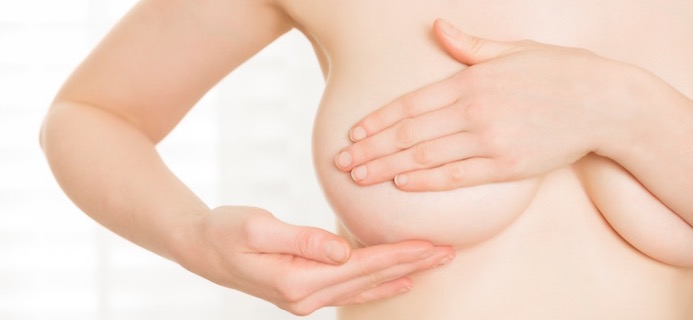
Each year, nearly half a million British women have lumps in their breasts checked out for cancer and hearteningly, nine out of ten turn out to be benign. But such lumps can be recurring and worrying – Alexandra Petra talks about her own experience and asks the experts about what can be done
I couldn’t argue with the distinct pea I found a little to the left of the nipple of my right breast one morning. I was following my own breast awareness ‘know what’s normal for you’ advice that I had written earlier that week for a glossy magazine.
That little lump of congealed something or other certainly wasn’t normal for me. It wasn’t gritty or hard like a marble but more like a ball of excessively hard cheese.
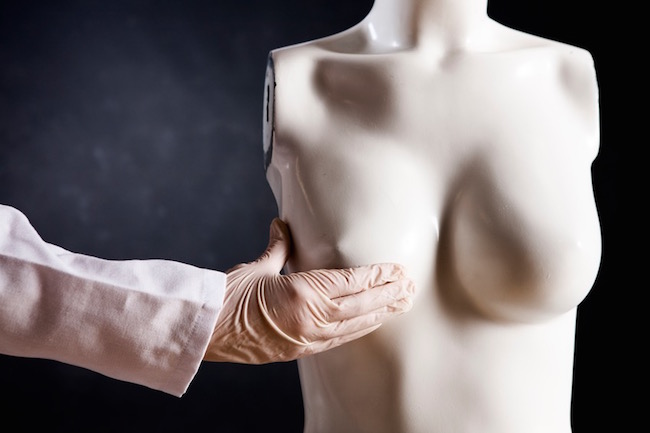
I went to my doctor who examined me, frowning and pressing hard into the fatty tissue of my breasts, nipples, underarms and collarbones. Along with the pea I’d found, he found another lump on the top right hand corner of the same breast. Yes they were certainly lumps, he said. But they were also smooth and mobile so probably nothing, but he would organise a mammogram anyway.
He got me – and my panic – into my local hospital’s breast care clinic for Monday. It was Friday.
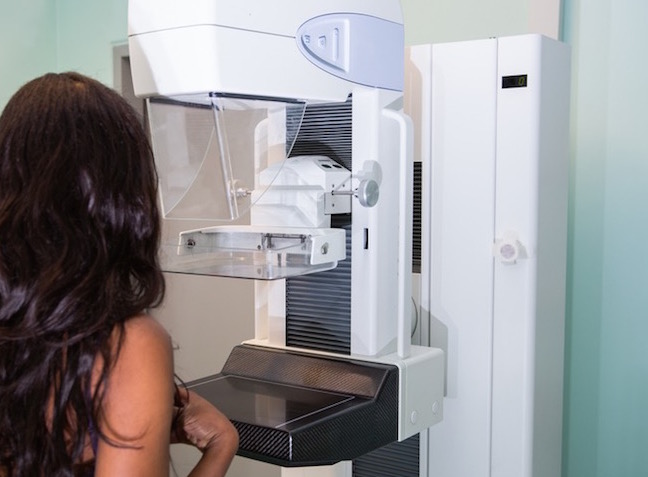
Gosh, mammograms hurt. Apparently, if like me you have small breasts it’s harder to see so they have to squeeze the bejaysus out of each boob between two cold steel plates until it is flat as a poppadom – I found it excruciating. I also needed an ultrasound because of the density of my breasts at 42.
MORE: It was like I was being stabbed in the breasts
‘Your breasts are full of cysts,’ said the radiologist. ‘But you don’t have cancer.’ Turns out I have a harmless but common condition that often strikes women in decades leading up to menopause. It’s called ‘fibrocystic breasts’ or lumpy breasts to you and me, and it can manifest as the cysts of various sizes in my breasts, which she pointed out to me on the screen.
‘Your breasts are full of cysts,’ said the radiologist. ‘But you don’t have cancer.’
She then inserted a fine needle into the largest one, the pea I had found, and within minutes I watched as six millilitres of light, greenish fluid quickly filled the syringe, making the lump disappear. There was no blood in it and it was transparent, both signs no further testing was required, the radiologist said.
MORE: Vaginal dryness: what you need to know
The words ‘don’t’, ‘have’, ‘cancer’ making me grin stupidly with relief, I put on my top, my sunglasses and walked out of the hospital. Since then though, I have found two subsequent lumps and both have turned out to be cysts – thankfully. Still, the mammograms are getting tedious and they continue to hurt like hell, leaving me wondering, what on earth can be done to help my naturally lumpy breasts?

A similar scenario plays out in 480,000 women’s lives each year. You find a lump. You freak out. You (hopefully) head straight for your GP. Like me, one in five women will regularly detect lumps and bumps in their breasts that turn out to be benign. The great news is, in nine cases out of ten that breast lump will be benign.
So how can we know? The truth is we can’t – and experts insist that any lumps that don’t feel normal to you should be checked out by your doctor. But here’s a peek into what he/she is thinking when they examine you.
Experts insist that any lumps that don’t feel normal to you should be checked out by your doctor
Firstly, a benign mass is usually three-dimensional, smooth, has regular borders and you can move it around under the skin. On the other hand, a malignant mass is usually firm in consistency, has irregular borders and may be fixed to the underlying skin or soft tissue and there may also be skin or nipple changes you can see.
MORE: The truth about bad breath
Either way, guidelines from the National Institute of Clinical Excellence (NICE) state that all breast lumps should be referred to a breast clinic for a mammogram (if you’re over 45), an ultrasound if you’re under 40 or in many cases, both.

BREAST LUMPS THAT AREN’T CANCER – A DOCTOR’S GUIDE
Dr Michelle Mullans, a consultant breast surgeon specialising in breast lumps at BMI Hospital, Droitwich Spa and NHS Worcestershire Royal Hospital explains
1. FIBROCYSTIC BREAST CHANGES
These are the most common form of lumps in women in their 40s and 50s, affecting one in four women.
Sometimes simply referred to as ‘lumpy breasts’, fibrocystic breast changes is an umbrella term that covers the differences in breast tissue caused by fluctuations in the hormones oestrogen and progesterone during a woman’s cycle and why such changes become more prominent at certain times in the month.
MORE: 10 health experts reveal the ONE item they would take to a desert island
There might be thickening, enlarging and general bumpiness, which often subsides post-period. Sometimes, they’re accompanied by pain (see 2) and sometimes not.
What can be done?
No specific treatment is necessary but if there is any kind of thickening or lumps that don’t subside after your period, you need to get it checked ideally mid-cycle by your GP.
2. BREAST PAIN
I see up to ten women a women a week panicking because of breast pain, thinking they have breast cancer but breast pain is common and cancerous lumps are not usually painful.

What can be done?
Start by getting out of underwire bras as these increase pain – sports bras or even maternity bras are not so sexy but better for breast pain.
Take ibuprofen orally or through an over-the-counter gel such as Voltarol. Gamma Linoleic Acid (see below) has been shown to help too but it it’s severe, Tamoxifen, a drug used to treat breast cancer, may be prescribed for six weeks to dampen down the pain cycle.
3. CYSTS
These are smooth, fluid-filled balls that form in the breasts that tend to be mobile and sometimes painful. They’re common and tend to appear in women aged 35-55.
As levels of oestrogen drop in the lead up to menopause, the body often responds by making a cyst. They become less common after a woman has reached menopause, but if she goes on Hormone Replacement Therapy (HRT) they may continue.
What can be done?
Your GP will refer you to a breast clinic where if you’re under 40, you would have an ultrasound scan (women who are under 40 usually have too much density in their breasts to be evaluated through mammogram).
If you’re over 40, you may have a mammogram and then be sent for an ultrasound which will immediately determine whether your lump is a cyst or something else.
If it is a cyst and it’s bothering you – perhaps it’s large or painful or both – the radiologist can do a ‘Fine Needle Aspiration’, in which a tiny needle is inserted into the breast by your doctor and the fluid, usually yellow or greenish is removed there and then with no anaesthetic.
If the fluid is not bloody and the lump disappears you won’t need further testing. But if the fluid is bloody or the lump doesn’t disappear your doctor may send the sample of fluid off for lab testing and refer you for further imaging tests and follow-up.
4. FIBROADENOMA
These develop because of an overgrowth of fibrous tissue in the breast that can form a solid lump again because of fluctuations in the hormones oestrogen and progesterone.
Most common in women under 40, fibroadenomas can also occur in women later though less frequently (I have seen one in an 80-year old).
What can be done?
A biopsy takes a few minutes and involves removing a tiny sample of the lump with a fine needle to be sent off to the lab for checking
If the patient is under 25 and the lump under three centimetres in diameter, no further treatment is usually necessary. But if she is over 25 or the lump is bigger, all such solid lumps need to be checked in which case the doctor would take a biopsy. This takes a few minutes – under a local anaesthetic, the doctor will remove a tiny sample of the lump with a fine needle and send it off to the lab for checking.
MORE: 6 ways to lose weight – by the A-list trainer
Once we know it’s a fibroadenoma, the woman can choose to have it removed surgically under a general anaesthetic, but this would leave a scar on her breast so many women choose to leave it alone – often advisable unless it’s increasing in size.
A new technique called a Vacuum Assisted Biopsy allows you to have the area frozen by local anaesthetic and the lump sucked out through a probe using a vacuum that leaves no scars – increasingly, breast clinics around the country are using it.
5. LIPOMA
These are little fatty lumps that can occur anywhere in the body including the breasts and are simply collections of fatty tissue.
What can be done?
Once the lump has been biopsied and confirmed as lipoma no further treatment is necessary unless a woman wants to have it removed, in which case it can be removed surgically (see fibroadenoma).
7 LIFESTYLE CHANGES PROVEN TO HELP
1. Go caffeine-free
Caffeine can be a trigger for breast pain and benign lumps. ‘Substances called methylxanthines in coffee green tea, cola and chocolate – the darker the variety, the more it contains – have been associated with benign breast lumps and pain,’ says Marilyn Glenville, a natural health expert and author of ‘The Natural Health Bible for Women’ (Piatkus £16.99).
‘They’re even present in decaffeinated tea and coffee.’

What to do: Reduce your caffeine (including decaf) by half over about four weeks and then half again until you’re caffeine-free.
A great caffeine free alternative to coffee is Barley Cup and to tea Rooibos tea (both from health food stores). Make them with a little milk to get that milky comfort associated with regular tea and coffee and you won’t even miss them.
2. Exercise (but keep it moderate)
‘A moderate amount of exercise has a balancing effect on hormones including oestrogen,’ says Glenville.
‘But keep it moderate as too much exercise may have the opposite effect’.
What to do: Opt for 30 minutes of walking, swimming, rowing, light resistance exercise or dancing five times a week.
3. Get into flax

There is a link between fibrocystic breast changes and constipation, says Glenville.
One study found that women who went to the loo less than three times weekly had four and a half times more breast problems than those who went daily.
‘This is about the body’s ability to eliminate excess oestrogen and progesterone from the liver,’ says Glenville.
‘When these hormones are not excreted through your poo, they will be reabsorbed by the body and could become a cause of benign breast lumps.’
What to do: Soak a tablespoon of whole flaxseeds (from the health food store) in a glass of water for half an hour and then at night before bed, swallow the lot with another glass of water as a chaser.
This can be done nightly as a natural alternative to laxatives, advises Glenville.
4. Try GLA

This stands for Gamma Linolenic Acid and is found in supplements such as Evening Primrose Oil, says Dr Mullans.
‘Taking GLA has been shown in studies to reduce the incidence of breast pain,’ she explains.
What to do: Take 1000 milligrams of Evening Primrose Oil a day and look on labels to ensure it provides about 100 milligrams of GLA – we like Healthspan’s Evening Primrose Oil 1000mg £14.95 from healthspan.co.uk.
5. Eat more lentils
Legumes such as lentils, chickpeas, soya and other beans and pulses contain substances known as phytoestrogens that can help block the activity of oestrogen receptors in our breasts that could be causing growth and stimulation leading to benign lumps and pain, says Glenville.

What to do: Look to international cuisines for legume inspiration, suggests Glenville.
For example, soya is a huge part of the Japanese diet (look for organic to ensure it’s not genetically modified), chick peas are a staple of middle eastern cooking and lentils are at the heart of Indian cuisine.
6. Eat more broccoli and cauliflower
Cruciferous vegetables have been shown to help metabolise excess estrogen in the body that could be contributing to benign breast problems,’ says Dr Nyjon Eccles, a medical and naturopathic doctor specialising in breast problems.
What to do: ‘Try and eat at least one serve of cruciferous vegetables such as broccoli, Brussels sprouts, cabbage, cauliflower, bok choi and kohlrabi daily and ideally raw or only lightly steamed,’ he advises (Kohlrabi is delicious sliced into chunky chips and eaten raw with a sprinkle of sea salt).
7. Take a test
If you get regular benign breast lumps you may have a condition known as ‘oestrogen dominance’ that leads to greater cell activity in the breasts and could result in problems such as breast cysts that recur throughout a woman’s life, says Dr Eccles.
What to do: Dr. Eccles and other good nutritionists and naturopaths can do an ‘oestrogen metabolism test’ costing around £150 done by testing your urine to measure how well your body is excreting excess hormones and advise on lifestyle measures to improve it.
Does having benign breast lumps increase my risk of breast cancer?
‘Having recurrent cysts, fibroadenoma, lipoma or breast pain doesn’t increase your risk of getting breast cancer,’ says Professor Louise Jones, breast cancer pathologist at Barts Cancer Institute, London.
Do an ‘oestrogen metabolism test’ costing around £150 done to measure how well your body is excreting excess hormones
‘But if you have fibrocystic breast changes they can come with cell proliferation and that can very slightly increase your risk of developing breast cancer, but the increase is very low – around 1.5 per cent.’
So should I still be having every lump I find checked out?
‘Every lump should really be checked out because a lump means a change,’ says Professor Jones.
‘Just because you have had nine cysts doesn’t mean you won’t ever have cancer. That’s not to scare you, but it’s simply to be cautious and safe.’
MORE: 9 ways to work mindfulness into your day
MORE: 12 healthy foods that look like the body part they’re good for
MORE: 5 summer beauty foods from the A-list makeup artist
Like this article? Sign up to our newsletter to get more articles like this delivered straight to your inbox.