Fiona Munro was diagnosed with ovarian cancer at the age of only 30, after months of visiting her GP with bloating. She was told she had an infection, IBS, or an STI. Then, all of a sudden, was diagnosed with stage four cancer and 12 months to live before surprising her doctors by going into remission. As part of Ovarian Cancer Awareness Month, Fi shares her story
Fiona Munro, 31, was a healthy businesswoman, career driven and making a life for herself in Scotland with her husband. But symptoms of bloating niggled away at Fi for years, but repeated trips to the GP were to no avail. With most diagnoses being in women over the age of 65 (53 per cent), consultants suspected Irritable Bowel Syndrome (IBS), allergies, an infection and even STIs. It wasn’t until her stomach had swollen to the size of a football and she was no longer eating that Fi was diagnosed with ovarian cancer and told she could have 12 months to live.
The UK has one of the lowest survival rates of ovarian cancer in Europe
Unfortunately, Fi’s diagnosis isn’t unusual. Almost half of women (45 per cent) wait three months or more from first visiting their GP to getting a correct diagnosis. These are statistics from Target Ovarian Cancer, leading the Start Making Noise campaign. They are focused on raising awareness of the symptoms, both amongst society and GPs, to increase survival rate.
Survival from ovarian cancer is much worse than for many other cancers, due to late diagnosis and a lack of effective treatment options. 4,100 women lose their lives in the UK each year – that’s 11 women every day, one of the lowest survival rates in Europe. There is positive news, however. According to Cancer Research UK, survival is improving and has almost doubled in the last 40 years in the UK.
As part of Ovarian Cancer Awareness month, Fi shares with Healthista her frightening story of diagnosis, but how cancer changed her life for the better. Don’t miss the symptoms at the bottom.
Fiona’s diagnosis
Fi, aged 30, sat in her car at the supermarket, about to go in and buy some bread when her phone rang – it was her consultant and he had the results of the tests. Only this time, he told her she needed to come in to hospital for the results, and bring her husband, Ewan. ‘I’d been speaking to this consultant nearly every day for two weeks and he always told me everything over the phone – although he didn’t confirm anything on the phone I knew things were no longer looking good and that my instincts had been correct’, recalls Fi.
Cancer – such a small word with such a huge impact.
It was 3pm when Fi and Ewan were shown to a private room in the hospital; Monday January 18th 2016, a date Fi will remember forever. ‘When the consultant arrived, he said, ‘you already know’. To which I replied, ‘yes, I have known for months’. Cancer – such a small word with such a huge impact. I looked to my husband, who I had been married to for two years, his face just a picture of stunned disbelief.

Fi was in stage four of ovarian cancer, the most serious stage, and medically she had 12 months to live. However, she had been suspicious of her symptoms for several years. In the five months leading up to her diagnosis, Fi had visited her GP six times and a consultant gynaecologist three times – and despite her bringing up ovarian cancer, remained undiagnosed. Almost half of women diagnosed (46 per cent) visited their GP a minimum of three months before getting a correct diagnosis, and over a quarter of women with ovarian cancer (26 per cent) are diagnosed through emergency services.
Fi had visited her GP six times and a consultant gynaecologist three times – and despite her bringing up ovarian cancer, remained undiagnosed
‘It was surreal, but I felt enormous relief. One of the first things I said to my husband whilst sitting in the hospital was ‘at least we can get a dog now’. I knew I would be at home and we have quite a dark sense of humour, which has kept us positive throughout this past year.’
MORE: 5 women-only cancers and how to spot their symptoms early
Knowing the symptoms
For a long time I believed I had IBS or a wheat allergy
Fi was well aware of the symptoms of ovarian cancer, despite less than a third of women in the UK confident they know the symptoms. ‘I’d been up during the night a lot to go for a wee, and so mentioned it to my GP, who said it was a hormonal issue from being on the Pill. I often got an upset tummy, so for a long time I believed I had IBS or a wheat allergy. I got a lot of hip pain and scans showed my left ovary was enlarged. I needed steroid injections for a while, but again, they believed it was hormonal.
‘I always Googled ovarian cancer over the years, wary that I had all the symptoms. But I was led to believe I was being paranoid or I was a hypochondriac, especially as on the NHS website it says that it happens to post-menopausal women.’
‘It wasn’t until I had an ectopic pregnancy in August 2015 that things became really out of hand’. An ectopic pregnancy is a complication in which the embryo attaches outside the uterus, ending a pregnancy. Fi had emergency surgery for internal bleeding, and in hindsight, says oxygen reaching her cancer cells would have made the cancer, already at stage two yet still undetected, spread more rapidly.
Emotional trauma from her ectopic pregnancy, infection from surgery, scar tissue, or to Fi’s horror an STI, were all suggested reasons for Fi’s cancer symptoms
In Fi’s ectopic pregnancy surgery recovery, she noticed severe abdominal bloating. ‘My sister was five months pregnant and we were the same size’, she recalls.
Emotional trauma from her ectopic pregnancy, infection from surgery, scar tissue, or to Fi’s horror an STI, were all suggested reasons for Fi’s cancer symptoms. ‘The first time I saw my gynaecologist consultant he wanted to test me for chlamydia. I said I had been with my husband for eight years so there was no chance. But he said ‘oh you’d be surprised’. I had a fear I had cancer, and someone was insinuating my husband had cheated on me. It was infuriating and a constant battle.’
MORE: 8 proven ways to prevent cancer

Fi continued her life, commuting to her work as a healthcare researcher two hours into Glasgow and back, running, lifting weights and seeing her personal trainer. It got to the point where Fi couldn’t carry on, in agony and not eating. ‘I remember lying on a sofa at work in so much pain. I decided to phone my consultant again. He asked me to come in and they checked my levels of CA125, which is a protein in the blood that can be a marker for ovarian cancer. They had done this before, and put the high levels down to an infection from the ectopic pregnancy surgery. Again, it had risen, but he still put it down to an infection.
I thought I was getting fat, but when they drained the fluid from my stomach I looked skeletal.
‘A few days later, I wasn’t eating at all. The swelling in my stomach was putting pressure on my organs, so they finally did an MRI scan and drained the fluid from my abdomen. It was five litres, and weighed five kilos. Where I thought, I was getting fat, I had actually lost so much weight I looked skeletal. They told me to go home while they tested the fluid, and I already knew what they were testing it for.’
‘I was a rare case aged 30’

A few hours later, Fi became one of 7,300 women diagnosed each year with ovarian cancer. According to the NHS, ovarian cancer mainly affects women who have been through the menopause (usually over the age of 50).
‘Being diagnosed stage four at 30 years old, without it being genetic, I was a rare case’, Fi said. ‘But my oncologist [doctor who treats cancer], told me it’s not as rare as people think; GPs and gynaecologists don’t expect to see it in a young person.’
As with all cancers, early detection and treatment is the key to survival. When a woman is diagnosed at the earliest stage, her chance of surviving for five years or more doubles from just 46 per cent to more than 90 per cent nearly half.
With a lack of women aware of symptoms, and GPs mistakenly believing symptoms only present in the later stages of the disease, it is perhaps not surprising that survival rates in the UK are among the lowest in Europe, according to Target. ‘My consultant said he was sorry’, said Fi. ‘But I don’t blame him at all. A lot of people ask me if am angry but I’m not. He followed the procedures.
‘My consultant said he was sorry’, said Fi. ‘But I don’t blame him at all.
‘When I had the surgery for my ectopic pregnancy, they weren’t looking for cancer. There is nothing that could have been done. However, if my GP and I had known there were more of a risk to young woman having it, I would have insisted even more than I did.
‘The only reason I got the scans in the first place was because I have a big personality, was persistent and not afraid to challenge the consultant’s decision, all whilst feeling I was fighting a battle and being dismissed. Whereas I think it could be fatal if young women are told they are fine and just accept it.’
MORE: 3 diet changes to lower your cancer risk
‘Chemotherapy was hell on earth’
From the moment Fi was diagnosed, her treatment began being discussed among her oncology team and she was introduced to her Macmillan nurses. ‘I wasn’t very shocked’, she said. ‘People around me were. I knew what I had been feeling inside, but some of them had joked I was just being paranoid in a reassuring way. The process of telling people that love you was harder than my diagnosis.

‘When you are diagnosed, you aren’t told your prognosis is unless you ask. When I had a chat with my oncologist I said ‘I don’t think I’m entitled to my life insurance, because I don’t think you are unless you are terminal.’ She didn’t answer. That’s when I realised how critical I was.’
Doctors originally thought Fi’s cancer was too severe to be operated on, already spreading to her lungs. However, by responding so well to chemotherapy, she had a 12-hour operation five months after diagnosis – the largest operation on a stage four patient in one sitting the doctors had done. They removed Fi’s cervix, womb, fallopian tubes, ovaries, appendix, spleen, diaphragm, part of her bowel, part of her liver, part of her pancreas, and part of the sack that keeps the organs in place (peritoneum). ‘They didn’t leave much!’ says Fi, who now has a colostomy bag.
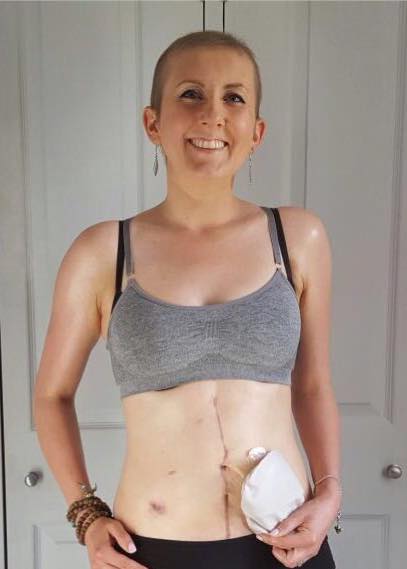
‘After surgery, I was in hospital on high dependency for four weeks’, Fi recalls. ‘When I was sent home, I was soon rushed back in an ambulance with a liver infection and sepsis (poisoning of the blood). That was my lowest point, I was out of it and hardly knew what was going on. And I still had more chemo to endure.’
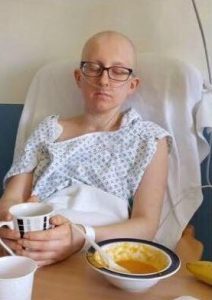
‘I am so lucky I had my husband to care for me a few days a week. I can’t imagine what it’s like for those going through chemo alone, like single mothers. Financially too, because we now rely on my husband’s wage, when previously I was the primary earner before. It’s frightening.’
MORE: What NOT to say to someone with cancer
‘Cancer made me re-evaluate everything’
When asked to summarise her year since diagnosis, Fi’s answer is far from what you would imagine. ‘Generally, last year was pretty good’, she says. ‘Most people think it’s really awful but actually it was really life affirming. I talk a lot about cancer as a gift. It sounds cliché, but having stage four cancer made me re-evaluate everything. I don’t stress about the little things anymore. You find out who your real friends are, and people who were acquaintances before became my best friends, and close relationships have fallen apart – that’s quite common.’
I talk a lot about cancer as a gift. It sounds cliché, but having stage four cancer made me re-evaluate everything.

Fi was told her cancer was incurable, and she had 12 months to live. But remarkably, she has been in remission since August. ‘My life insurance never paid out and my oncologist can’t sign the paper work to say I have 12 months to live. They can’t project beyond 12 months so they either say you’re going to die in 12 months or you will live longer. So now, I’m sitting in the ‘live longer’, which makes me very happy. I know a time will come when she says it’s less, but it’s a nice reminder to just live in the moment.
Everyone is terminal. The only thing with cancer is you are more aware of it
‘Something I tell myself a lot is that everyone is terminal. The only thing with cancer is that you are more aware of it. I think we stumble through life thinking we have forever, but actually, you can be hit with a life shocker at any stage. I have a limited time and I base my decisions on that – it would be nice if everyone could live like that.’
MORE: How breast cancer saved me from workaholism
Yoga and meditation kept Fi positive and active through her treatment, and now she is feeling better, she is trying her hand at being a businesswoman. Already finished a yoga teacher training course, Fi has started running classes across Scotland, for both adults and in schools and nurseries to improve children’s wellbeing.
Fi was told her cancer was incurable, and she had 12 months to live. But remarkably, she has been in remission since August

‘I don’t have the commute or stress of work anymore. It’s totally different to how I was before – I was always career driven and obsessed with succeeding, whereas now success means to me being happy and looking after yourself. It’s not about money or statement.’
Don’t miss the symptoms
Target Ovarian Cancer outline the symptoms to look out for:
- Persistent pelvic or abdominal pain (that’s your tummy and below)
- Increased abdominal size/persistent bloating – not bloating that comes and goes
- Difficulty eating or feeling full quickly
- Needing to wee more urgently or more often than usual
Occasionally there can be other symptoms such as changes in bowel habits, extreme fatigue (feeling very tired), unexplained weight loss or loss of appetite. Any post-menopausal bleeding should always be investigated by a GP.
Symptoms will be:
- Frequent – they usually happen more than 12 times a month
- Persistent – they don’t go away
- New – they are not normal for you and may have started in the last year
To find out more, click here.

Follow Fi’s journey on her blog, Facebook, Twitter and Instagram
Do you have an inspiring story you would like to share? Let us know by tweeting @HealthistaTV
READ MORE
What to do about breast lumps (that aren’t cancer)
What is lupus? Three women describe living with a disease that can attack the entire body
The truth about caesarean sections – a doctor’s guide
Like this article? Sign up to our newsletter to get more articles like this delivered straight to your inbox.





















































