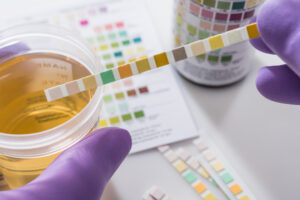
Over 20 per cent of people in the UK live with some form of bladder complaint. Here are 3 common bladder problems and what you can do to treat them
Bladder weakness, cystitis and urinary tract infection are common bladder problems that can make you too embarrassed to seek help.
Around 14 million people in the UK live with some form of bladder complaint (NHS England, 2023).
That’s over 20 per cent of the population, with twice as many women affected as men.
14 million people in the UK live with some form of bladder complaint
‘If you’ve got a bladder problem, you may feel embarrassed, isolate yourself, or limit your work and social life,’ says Sharon Hamilton, Registered Nurse and Incontinence Advisor for Molicare.
‘You may also avoid physical and leisure activities. But, don’t let embarrassment stop you from getting the right help. No matter what your issue, there is always help available.’
#1 Cystitis and UTI’s
One in three women will experience a urinary tract infection by age 24, and almost half of women will have one in their lifetime (Translational Andrology and Urology Journal, July 2017).
‘Urinary tract infections (UTIs) are most often caused by bacteria and affect the urinary tract, including the bladder (cystitis), urethra (urethritis) or kidneys (kidney infection),’ says Gynaecologist Tania Adib, London.
‘Typical symptoms may include pain or a burning sensation when peeing (dysuria), needing to pee more urgently and frequently than usual and urine that looks cloudy, dark or has a strong smell.
‘You may also feel pain in your tummy or lower back, feel feverish and shivery and there may even be blood in your pee.’
One in three women will experience a urinary tract infection by age 24
‘Cystitis is a UTI that affects the bladder. It affects more women than men and is one of the most common complaints seen by GPs,’ says Tania.
‘Typical symptoms are urgency, pain, discomfort and a burning sensation when you pass urine. It’s normally caused by a bacterial infection that enters the bladder via the urethra.
‘Women have a shorter urethra than men which makes it easier for bacteria to cause an infection.
‘For example, if you’re sexually active, use tampons, or by the hormonal changes that occur due to menopause (when the lining of the urethra becomes more sensitive).’
How to treat cystitis…
Talk to your your GP who will arrange a urine test. You may be given a prescription for antibiotics. But, in many cases symptoms often resolve with self help tactics.
‘If you’ve haven’t got enough healthy bacteria in your gut, this lowers immunity and can make you more prone to urinary tract infections such as cystitis,’ says Tania.
Research shows that specific probiotic such as lactobacillus rhamnosis and lactobacillus reuteri bacteria can inhibit the growth of bad bacteria commonly leading to UTIs.
Try: Viridian Synerbio Lactobacillus Rhamnosus GG, ethical and pure supplements with no fillers or preservatives in, £22.60.
What’s more, research shows that D-mannose and cranberry can inhibit bacteria that causes UTIs.
Try: Cytoplan D-Mannose vegan powder, £32.60 for 50g – contains D-mannose, a natural (non-glycaemic ) plant sugar.
Here are some other things you can do:
- Drink plenty of water to flush out your system.
- Drink 2 tablespoons of apple cider vinegar with water, twice a day to alkalise your system.
- Always go to the toilet immediately after sex.
- Take an OTC preparation to alleviate symptoms.
- Take a daily probiotic.
Try: CanesOasis Cystitis Relief – a cranberry flavoured remedy that contains sodium citrate, to reduce acidity.
#2 Bladder Weakness & Incontinence
Do you dread coughing, laughing or sneezing, because you might wet yourself?
‘Bladder weakness and urinary incontinence affects one in four women in the UK,’ says Sharon Hamilton, Registered Nurse and Incontinence Advisor for Molicare.
‘There are two main types of bladder weakness. The first is stress incontinence, which happens when physical movement or activity, such as coughing, laughing, sneezing, running or heavy lifting, puts pressure (stress) on your bladder, causing you to leak urine.
‘Stress incontinence is caused by weak pelvic muscles and may occur if muscles are weakened (or damaged) after giving birth, during pregnancy, or if you are overweight, and getting older.
Bladder weakness and urinary incontinence affects one in four women in the UK
‘If you have stress incontinence, you may feel embarrassed, isolate yourself, or limit your work and social life. You may also avoid physical and leisure activities.
‘With treatment, you’ll likely be able to manage stress incontinence and improve your overall well-being.’
‘Then there’s Urge (urgency) incontinence is the unintentional loss of urine,’ Sharon adds.
‘If you have urge incontinence your bladder muscle contracts, causing a sudden urge to urinate before you can get to the bathroom.’
Common causes may include: drinking too much alcohol or caffeine, not drinking enough fluids, so urine to become too concentrated and irritates the bladder, constipation, certain medicines, neurological conditions, UTIs or tumours in the bladder.
How to treat incontinence and bladder weakness…
If you are experiencing bladder weakness or incontinence, always talk to your GP who will assess your condition.
Keep a bladder diary for a few days before your appointment – eg: how often you experience leaks etc. This will help to provide as much information as possible.
You may also have tests to rule out any underlying causes. Your GP can also refer you to a nurse or pelvic physiotherapist who deals with bladder problems.
READ MORE: Pelvic Floor FAQ’s – here’s what you need to know
Pelvic floor muscle training
‘Physiotherapists, doctors and nurses know that exercising the pelvic floor muscles can help to improve your bladder control,’ says Sharon.
‘When done correctly, pelvic floor muscle training exercises can build up and strengthen these muscles and so help you to control your bladder.’
Here’s a simple exercise to try:
- Slowly tighten bladder muscles as hard as you can.
- Hold for 5 seconds.
- Repeat 5 times.
- Practice 6 to 10 times a day.
For more exercises – https://apps.apple.com/gb/app/kegel-trainer-pfm-exercises/id578148339
Lifestyle Changes
Keep a bladder diet diary. This will help you to see what any correlation between certain foods and symptoms.
According to advice from Bladder Health UK (bladderhealthuk.org) certain foods can irritate the bladder, making symptoms worse.
Foods to avoid include:
- Tomato based and highly spiced foods,
- fruit and fruit juices,
- fizzy drinks,
- caffeine,
- alcohol,
- tea and coffee,
- artificial sweeteners,
- soy products,
- yeast,
- highly preserved meats,
- fish and fast food can be irritants.
Try: Healthspan’s New Bladder Support With Go-Less, £19.95 for 60 capsules.
This new supplement is a blend of plant extracts made from soy germ and pumpkin seeds, and a specific process called EFLA® HyperPure Production is used to extract the pumpkin seed to retain its efficacy and purity. pumpkin seed, vitamins B6, D3 and zinc to help support normal urinary flow.
Go-Less® is clinically researched with 4 published human clinical trials that demonstrate that Go-Less® is safe and has positive effects on urinary bladder function for both men and women.
READ MORE: The new shorts that helped this woman’s urinary incontinence
Watch your weight
‘Being overweight can weaken your pelvic floor muscles and cause incontinence because of the pressure of fatty tissue on your bladder,’ says Sharon.
‘Symptoms may improve, and could go away completely, if you lose excess weight.’
In one study (New England Journal of Medicine, 2009) overweight women who lost on average 17lbs of body weight had a 47 per cent reduction in weekly incontinence issues.
Keep stress under control
‘Some women who struggle with anxiety and depression also struggle with incontinence,’ says Sharon.
‘It can go both ways – mental stress can cause incontinence, and incontinence can also cause mental stress. Mental health conditions, such as anxiety and depression, are common among people with incontinence and overactive bladder (OAB), but pelvic floor exercises, yoga, and treatment may help manage it.’
mental stress can cause incontinence, and incontinence can also cause mental stress
You might also benefit from counselling or CBT (cognitive behavioural therapy) alongside treatment
Choose the right products to keep you dry
Using incontinence products (eg: absorbent pants or pads such as, Molicare Premium Lady Pad, £1.99 for 14 pads) can be helpful while you’re waiting to be assessed or receive treatment and struggle there are products to help you on the market at this difficult time.
READ MORE: From menopause to UTI symptoms – a Doctor’s Guide to everyday women’s health concerns
Surgical Treatments
There are a number of treatments for incontinence, where lifestyle and other interventions are not enough.
These include surgical interventions such as sling surgery (where a tissue sling is placed around the neck of the bladder to support it), vaginal mesh (where a synthetic mesh is inserted behind the urethra to support it) and colposuspension (surgical bladder lift). Your GP will advise you on your best options.
#3 Over active bladder syndrome (OAB)
‘This is where you feel an urgent need to go to the toilet more than eight times a day,’ says Pelvic Physiotherapist, Elaine Miller (gussetgrippers.co.uk).
‘Often it’s to do with feeling anxious about having an accident, so you start to go to the toilet more often. But, after a while your bladder capacity starts to reduce.
with OAB, the bladder muscle becomes overactive and contracts when you don’t want it to
‘Normally, we get the urge to go when the bladder is half full. But, with OAB, the bladder muscle becomes overactive and contracts when you don’t want it to.’
How to treat OAB…
- Avoid caffeine and alcohol.
- Ask your GP to refer you to a pelvic physiotherapist for bladder training.
- Practice pelvic floor exercises.
- Reduce stress as this can make OAB worse.
Like this article? Sign up to our newsletter to get more articles like this delivered straight to your inbox.