Sjogren’s Syndrome is an autoimmune disease few of us have heard of – Elif Mazi certainly hadn’t until she was diagnosed with it at just 20
I don’t know if you’ve ever tried Happy Hippos but it’s a sweet snack produced by popular chocolate company Kinder. It’s got a wafer coating, cream in the middle, and little white flakes for decoration. I was sitting at a table at university, aged 20, nibbling on a Happy Hippo when I felt like one of the flakes had got stuck under my tongue.
At this point I just wiggled my tongue around to try and swallow the flake but the sensation that it was stuck wouldn’t go away. This is when I decided to investigate. It wasn’t a painful sensation, but rather simply uncomfortable.
Imagine a tiny balloon made up of your own skin just sitting on the floor of your mouth – that’s exactly what I saw the mirror
I whipped out my pocket mirror and checking to locate and fish out the flake. Under my tongue there was no flake but rather a ball of flesh on the floor of my mouth.
I freak outed out. Immediately showing my two friends and asking for their advice didn’t help. They both thought it was gross and wanted me to close my mouth. We concluded that if it’s still there in a few weeks, I’d go to the doctor about it.
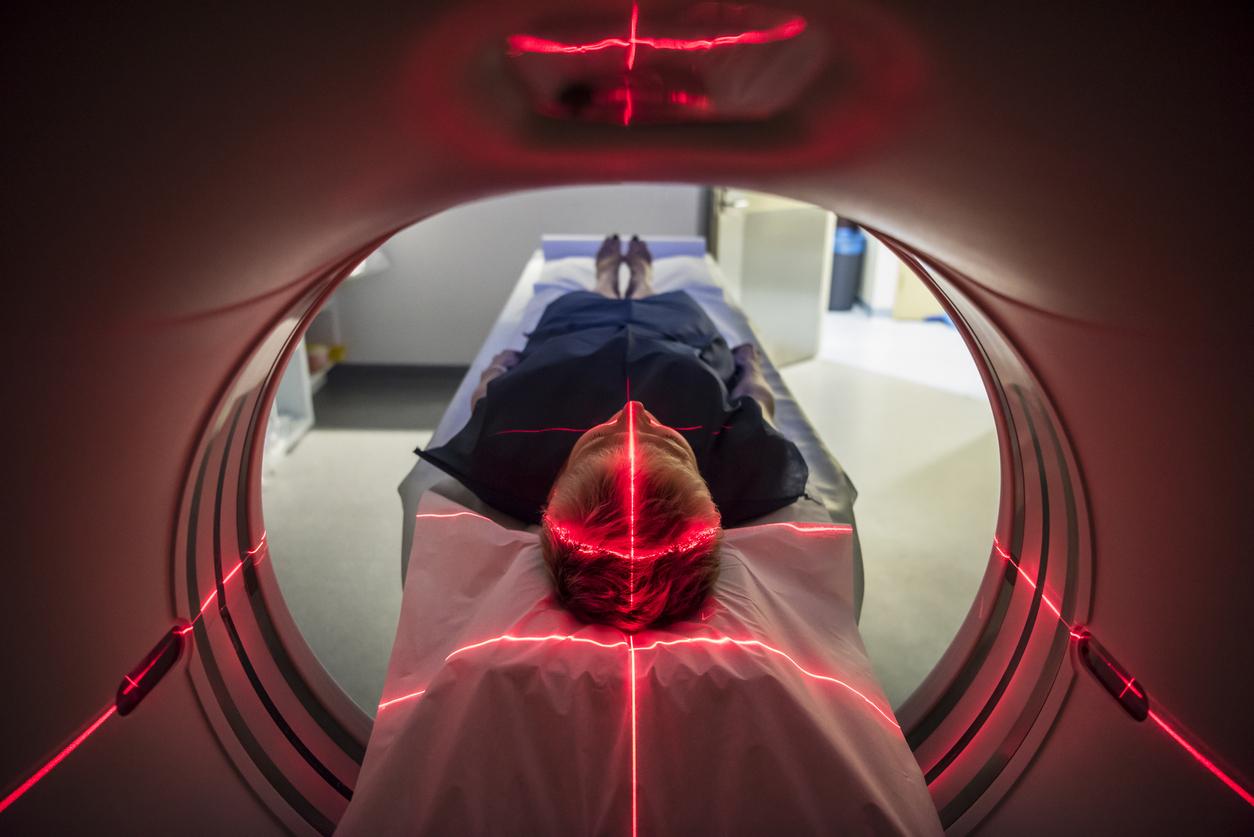
Eventually I end up at the GP for my mouth flesh ball that wouldn’t go away, opening my mouth up wide and waiting patiently for any sort of verdict. Over the course of several weeks and months I did a series of tests and scans at hospitals, one of which was an MRI.
During an MRI, a human body slowly slides into a closed machine while a doctor stares from a big window. Well, that’s basically what it’s like. I was told I was only going to be in there for around fifteen minutes, but by the end I was asked whether I could stay in there for a bit longer as the doctor wanted to check something else.
Up until this point the multiple doctors I had seen concerning the ball in the mouth (which I later found out was a benign cyst, and simply a clogged salivary duct that had saliva trapped in it) hadn’t thought the cyst was linked with anything else.
This may be true, but Dr. Elizabeth Price who is a consultant rheumatologist at the Great Western Hospital and is the medical president and trustee of the British Sjogren’s Syndrome Association (BSSA), suggests otherwise. Turns out, those who have Sjogren’s produce thicker saliva than others. So perhaps my clogged salivary gland wasn’t just a random occurrence after all?
Back to the MRI scan, after staying in there for an extra ten minutes or so, I get dressed and go home. When I see my doctor next, he tells me that the person controlling the MRI scan picked up on some abnormal behaviour on my parotid gland. This is located along the side of the face near the ears and is a type of salivary gland.
that flesh ball was a clogged salivary gland, because those who have Sjogren’s produce thicker saliva than others
He immediately goes on to say that he suspects I may have Sjogren’s syndrome, and requests that I do some more tests to figure out whether I have the illness or not.
In that moment I was confused and not sure how to react. My mother and I begin bombarding the doctor with questions. What is it? Where did I get it from? Is there a cure?
Some time later, after doing a specific blood test to check how many white blood cells I had, it was confirmed that I have Sjogren’s. Though it was still mild and thankfully didn’t affect my life too drastically, I was lucky enough to get diagnosed early on – most people are not diagnosed for years.
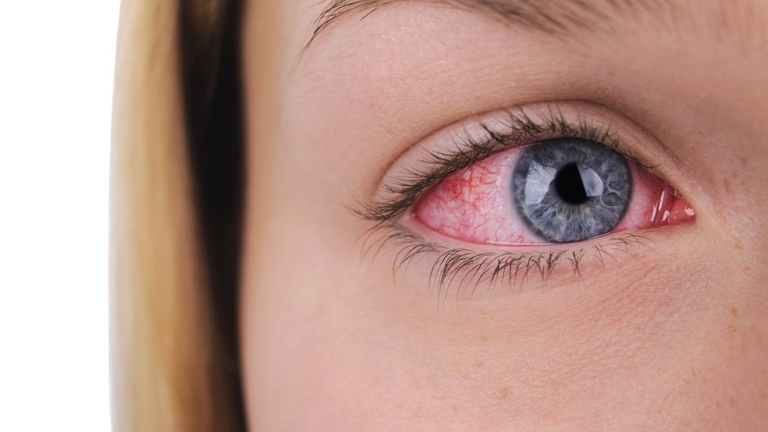
Almost two years on, I’m lucky to say that my symptoms aren’t too bad. When I sit in front of my computer everyday, my eyes get tired and dry a lot more than most people’s. I haven’t needed to use any supplements or medication for it yet, and a simple massage around my eyes does the trick for now.
One of my main concerns when being diagnosed was that because I was diagnosed so young, I assumed that with time the illness would get worse.
Dr Price, however, told me that increasing evidence shows that this disease tends to be a chronic low level one that doesn’t change. Basically, statistically my Sjogren’s shouldn’t get worse – but only time will tell what happens.
Since then I’ve been slowly trying to improve my diet by eating more nutritiously and exercising. This whole experience has taught me to care for my health before it could be too late.
What is Sjogren’s syndrome?
So how would a specialist define it? Dr Elizabeth Price defines the syndrome as a ‘chronic rheumatic disease which creates dryness in the eyes and mouth, aches and pains and fatigue.’
You’re probably wondering, ‘if dry eyes are such a problem, can she cry?’ Well, people with harsher symptoms than me are unable to cry as much but luckily, while I can still cry when I’m sad, my eyes feel very dry afterwards.’
Because the main symptoms of Sjogren’s seem innocuous – dry mouth, dry eyes and fatigue – the disease can be easily brushed off not only by those suffering from it but many doctors too. After all, many of us have dry eyes from staring at our phones and screens too long.
In fact, the UK Primary Sjogren’s Syndrome Registry which collects data on people with Sjogren’s across the UK reports that the average diagnosis takes around eleven years. So, most people with the illness will have symptoms of it for ten or eleven years before they are officially diagnosed.
Often times dentists are the ones fishing out the possibility of Sjogren’s in someone, as the lack of saliva means those with the disease have faster decaying teeth than those who don’t.
the lack of saliva means those with the disease have faster decaying teeth than those who don’t.
Some women may also experience a drier vagina due to this illness. Moisture-producing glands are at risk and the vagina, eyes and mouth are the most common to be attacked.
You might be thinking that oh, it’s just a bit of dryness, what harm will it do? But some people have lost their teeth over time because of it and the fatigue can prevent you from going about your daily life, depending on how bad the illness is affecting you.
This illness goes beyond dryness and fatigue, however. Aches and pains, skin rashes, and possibly anaemia or low levels of white blood cells can also be a part of it.
What triggers Sjogren’s syndrome?
There is no direct cause as it is an autoimmune disease, meaning its origins come from within the person affected. Though there aren’t clear answers as to why autoimmune diseases exist and who they affect, Price says, ‘some people have a genetic vulnerability to it.’
This doesn’t mean your relatives have the same autoimmune disease, however. Some either have completely different ones or none whatsoever.
The direct cause is unknown, says Dr Price. ‘It’s thought that something triggers it – and this could be a combination of factors – but what these triggers are, however, is unclear,’ she explains.
As Sjogren’s in particular is seen in women, one of the triggers could be hormonal or there may even be viral triggers – but again, this is mostly guesswork.
One thing scientists do know is that people with Sjogren’s tend to have a higher amount of specific antibodies known as antinuclear of ANA antibodies and doctors will usually test to see how much a patient has to determine which of us is more likely to get complications from the illness.
Am I at risk of having Sjogren’s?
So who does it typically affect? Women aged 40-60 are usually the ones getting diagnosed for Sjogren’s, though of course the illness isn’t limited to those ages or gender.
Because of this lack of knowledge, there isn’t much people can do in order to prevent it. There is no cure but there are still a few things you can do in order to prevent it from worsening (see below).
It’s also interesting to note that some races might even be more prone to the illness than others. Dr. Price says that most autoimmune diseases are slightly more common is those of Asian descent.
How to help the symptoms of Sjogren’s syndrome
One thing’s for certain, according to Price. Smoking has a negative effect on most autoimmune diseases so that’s a big no no.
Drinking water is probably the first thing a rheumatologist would tell you to do. Then, there are artificial tears and saliva you can use. Eye drops are also heavily recommended by doctors, as long as they are preservative free.
If you wear contacts, switch to glasses instead. Contacts can cause even more dryness in your eyes and try to avoid excessive screen use too.
Diet and lifestyle changes can really influence how much the illness impacts your life. By living a healthier lifestyle and including omega 3 and 7 fatty acids into your diet (especially those found in oily fish), the syndrome may be easier to handle.
That being said, avoid omega 6 fats as much as possible as they encourage inflammation. These are found in processed foods and vegetable oils and most Western diets are quite rich in it.
Dr Price suggests staying at a ‘sensible weight’ and keeping your environment moist. Avoid air conditioning too as this only exacerbates the problem.
There is also an idea that going gluten free is great for autoimmune diseases. Dr Price says that though there isn’t direct scientific evidence for this, she has come across several people with autoimmune diseases who claim it’s helped their symptoms.
Now, because the disease affects the moisture producing glands, massaging where your glands are located could help.
You can also use artificial tears and saliva as a replacement, if they are preservative free.
There are of course some medication that can be used too. Pilocarpine is used to treat pressure of the eyes and mouth that patients can sometimes feel from a lack of tears and saliva. ‘It’s an old-fashioned drug that stimulates secretion’, says Price.
How to get diagnosed/tested
It’s important to go to your dentist and optician regularly. There, they can tell you the level of moisture which your glands are producing.
When getting your eyes checked, you can ask for a Schirmer’s test. This is when your eye doctor will measure how much moisture your eyes produce by placing strips of paper on the bottom of each eyelid.
On top of this, if your optician has the equipment, they can check to see how much of your tear film has been damaged by having dry eyes – which can help test for Sjogren’s syndrome.
Will my children have it? Am I likely to get other diseases?
There’s also no evidence showing that if you have the illness your children will have it too, though if you have Sjogren’s, doctors will take extra precautions to make sure your baby is okay throughout your pregnancy.
However, there are two main rare complications that could be seen in newborns – though they are unlikely and only five in 100 women who carry the positive antibodies will be affected. Firstly, your baby could get a skin rash that looks like a lupus rash. This is because the antibody found in Sjogren’s is small enough to get to the placenta filter and into the baby’s circulation which means the baby ends up with your antibodies in their system. It’s important to note that these rashes can also be sun-sensitive.
By 22 weeks if the heart rate of the baby is normal, your child will be fine. But, if not, your pregnancy will need to be monitored carefully.
The other possible complication, which affects less than one percent of babies is some complications in the baby’s heart. ‘A normal baby’s heart rate is at around 140’, says Dr Price. ‘And in the baby’s affected in these cases their heart rate is 48’.
It’s important to get an early booking with doctors as early as you can so they can give you a detailed ultrasound scan between 17 and 22 weeks. This is when doctors can pick up the heart rate of the unborn child. By 22 weeks if the heart rate of the baby is normal, your child will be fine. But, if not, your pregnancy will need to be monitored carefully.
So, though your future babies might not be born with it – there is still a risk that they might develop it later on in life.
One important thing to mention is that typically with autoimmune diseases, if you’ve got one, your chances of getting another one are higher.
Rheumatoid arthritis, lupus and thyroid disease are often more common in those with Sjogren’s. In fact, it’s believed one in five people with Sjogren’s will also develop thyroid disease.
A vitamin B12 deficiency can also occur, so it’s important to look out for that.
Though thyroid disease is common, it’s easily treated. After getting your thyroid function checked every year or two, you can get thyroid replacement medication to help.
A study on 24 female Sjögren`s syndrome patients aged 37-66 randomly took an Omega 7 supplement or a coconut oil capsules (as a placebo). They took six capsules per day of each product for three months.
Twelve typical symptoms of Sjögren`s syndrome, dry eyes, mouth and genital tract and the skin were evaluated using a visual analogue scale (VAS) before and after each of the supplementation periods.
The use of the Omega 7 supplement led to a higher percentage of improved cases in all the twelve symptoms followed by the study. Try PharmaNord’s Omega 7 capsules, £19.95.
For more information about sjogren’s and other autoimmune illnesses you can go to rheumatology.org and the British Sjogren’s Syndrome Foundation
More Healthista Content
8 signs you might have coeliac disease that might surprise you
What is omega 3, 6, and 9 and which ones do you REALLY nead?
3 things this TV Doctor wants you to know about healthy weight loss
10 best supplements for vegans
Like this article? Sign up to our newsletter to get more articles like this delivered straight to your inbox.