Love Island newbie Rebecca Gormley entered the show with a visible contraception patch, leaving people wondering whether there is a better option of contraception out there than the popular Pill. We evaluate four contraception alternatives
Who’s watching the new winter series of Love Island? Well we certainly are, #bodygoals and all that.
If you are a Love Island fanatic, then you would have noticed that new girl Rebecca Gormley (and former Miss Newcastle) entered the villa by storm, which aired Monday evening at 9pm.
She not only caught the boys attention but the girls too, with contestant Shaughna Phillips saying Rebecca had the ‘hair of a goddess’.
Read more: 7 easy hair growth tips for long, luscious locks
Beady eyed viewers also noticed how drop dead gorgeous the new 21-year-old bombshell was, but something else caught their eye too – a visible patch on the top of Rebecca’s right leg.
Viewers noticed what seemed to be a contraceptive patch on her thigh during Tuesday night’s episode when Rebecca was on her dates in the Hideaway with fellow contestants, Callum Jones and Connor Durman.

Viewers praised the beauty queen for her sexual health and safety precautions, and we can’t help but love the contraception representation too!
But many viewers were completely unaware that the contraceptive patch was even a thing.
The contraceptive patch, known as the Evra in the UK is a small, sticky patch that prevents pregnancy by releasing hormones into your body.
It works in the same way as the combined contraceptive pill, and is more than 99 per cent effective when it comes to preventing pregnancy. It does not however protect against STIs so condoms are still necessary when having sex.
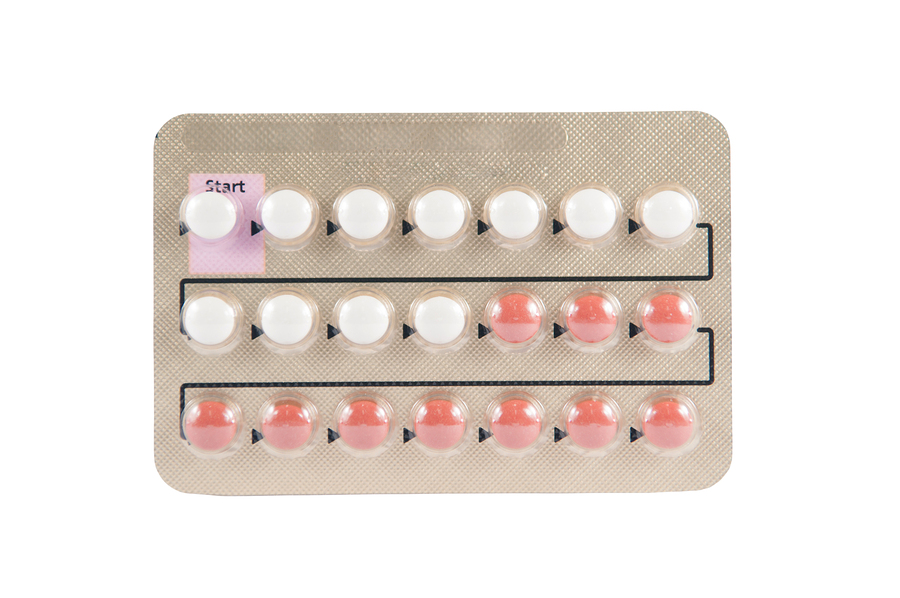
The most popular contraceptive choice – the Pill
Four million British women take the Pill.
Although it comes in 23 different types, many still struggle with it and live with horrendous side effects including headaches, nausea and mood swings along with physical changes to their bodies such as weight gain.
‘Some women complain of being spotty or moody,’ says Dr Anne Connelly, a GP at The Ridge Clinic in Bradford and chair of the Primary Care Women’s Health Forum.
‘Some people say they’re putting on weight or feel bloated. There’s no doubt some of the Pills have more side effects than others.’
Some family planning experts such as Connolly are now urging women to consider newer forms of fit-and-forget contraception that require no daily popping.
Although the Pill has its cons, it also has a pretty massive pro – that is that it can prevent certain types of cancers in women.
Indeed, a landmark study revealed that the Pill can help prevent certain cancers in women.
According to research conducted by the Royal College of General Practitioners, women who have used the pill at any point in their life are less likely to get ovarian, endometrial and colorectal cancer. They also found no evidence that taking the Pill increases risk of developing other cancers.
The results of the study are an amazing discovery, but it doesn’t necessarily mean you should go running to the pharmacist just yet.
What are contraception alternatives to the Pill?
Of the 15 different types of contraception available in Britain, only one is the Pill, and according to a recent study, one in five women didn’t know what alternatives were available to them.
Moreover, a staggering three quarters had never had a conversation about non-Pill contraceptives with their doctors.
A group of contraceptives called Long-Acting Reversible Contraceptives (LARCs) not only require no need for a daily pill, but they are also more effective, says Connolly.
‘LARCS are 99 per cent effective whereas the Pill has an 8 per cent failure rate,’ she explains.
‘But what we’re finding is doctors aren’t taking the time to tell their patients about their non-Pill contraceptive options,’ she says.
‘The Pill has done some great things for women in the last 50 years, says Professor John Guillebaud, emeritus professor of Family Planning at University College London and author of The Pill and Other Forms of Hormonal Contraception (Oxford University Press £9.99 from Amazon).
‘But when it comes to the next half century, women should be looking at the new contraceptive methods available to them, especially the long-acting reversible contraception options such as the 3-year implant in one’s upper arm or the intrauterine system that usually makes periods lighter and pain-free,’ he says. ‘In my opinion, the latter is the greatest advance in birth control since the invention of the Pill’.
Here’s a rundown of the LARC options available free from your GP…
The Patch aka the Evra patch
PROBLEM: ‘I get heavy, painful periods’
TRY: The Evra patch
The contraceptive patch is a small sticky patch that releases hormones into your body through your skin to prevent pregnancy. In the UK, the patch’s brand name is Evra.
The contraceptive patch releases a daily dose of hormones through the skin into the bloodstream to prevent pregnancy.
It contains the same hormones as the combined pill, (oestrogen and progestogen) and works in the same way by preventing the release of an egg each month (ovulation).
It also thickens cervical mucus, making it more difficult for sperm to move through the cervix after sex. The womb lining is thinned so a fertilised egg is less likely to be able to implant itself.
When used correctly, the patch is more than 99 per cent effective at preventing pregnancy. Each patch lasts for one week, before needing to be changed for a new one. You change the patch every week for three weeks, then you can have a week off without a patch.
You don’t need to think about taking something every day like you do with the pill, and it’s still effective if you’re sick or have diarrhoea. Plus you don’t have to worry about taking it on and off before entering water as it is waterproof. You can wear it in the bath, when swimming and while playing sports.
Advantages of the patch:
- The patch has also been said to protect against ovarian, womb and bowel cancer.
- Easy to use and doesn’t interrupt sex.
- Unlike the oral contraceptive pill, you don’t have to think about it every day, you only have to remember to change it once a week.
- The hormones from the patch aren’t absorbed by the stomach, so it still works if you throw up or have diarrhoea.
- It can make your periods more regular, lighter and less painful.
- It may reduce the risk of fibroids, ovarian cysts and non-cancerous breast disease.
Disadvantages of the patch:
- The patch can raise your blood pressure, causing headaches in some women.
- The patch does not protect against sexually transmitted infections (STIs), so you may need to use condoms as well.
The Mirena (also known as the IUS and the coil)
PROBLEM: ‘I get heavy, painful periods’
TRY: The intra-uterine system or IUS
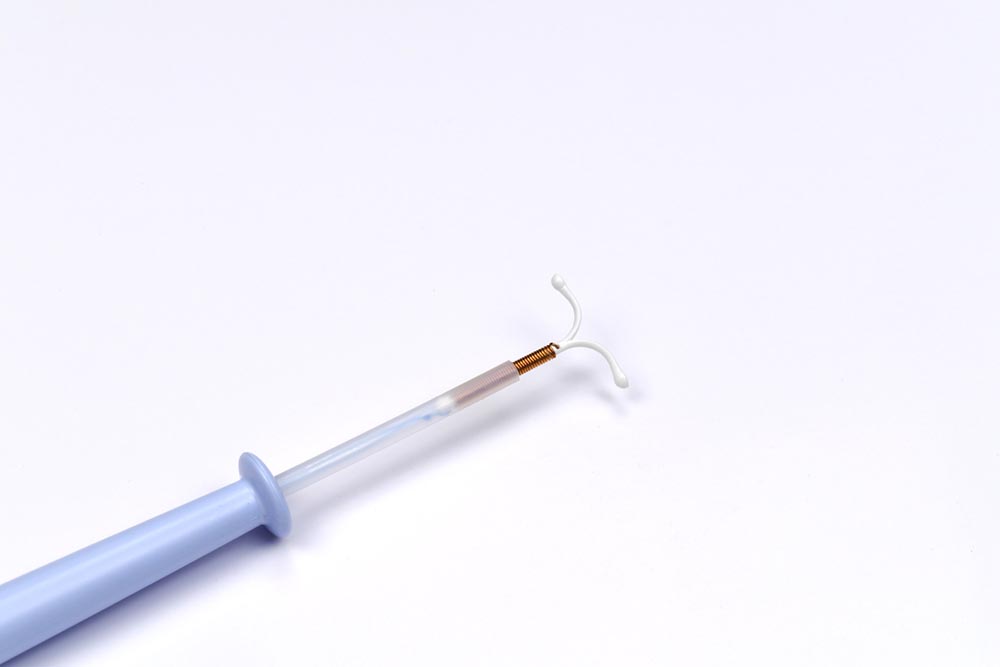
The ‘Mirena’ or Intrauterine system IUS is a small T-shaped plastic device inserted into the uterus by a doctor where it releases the hormone progestogen.
It secretes small amounts of the hormone progestogen into the womb, which thickens cervical mucus making it difficult for sperm to move through. It lasts five years.
Pros Fertility returns to normal after it’s removed. Periods can become lighter, shorter and less painful. Dr Connolly says you can have a 90 per cent reduction in period blood loss in a year. Because it’s action is local, less hormone enters the blood stream so side effects are usually minimal.
Cons If you haven’t had children or your doctor has little training, insertion can be painful so ask for a local anaesthetic and make sure you go to someone with experience inserting it – if your GP hasn’t fitted many of them go to your local contraceptive clinic instead.
You might get breast tenderness, acne and headaches, irregular bleeding and spotting, though these usually subside after six months.
The implant
PROBLEM: ‘I get moody’
TRY: The implant
The ‘Nexplanon’ is a tiny hairpin-sized rod put into the skin of the upper arm where it releases progestogen for three years.
‘The progestogen hormone in the implant is less mood-causing than the other forms,’ says Dr Connolly (the copper coil may also help if you have hormonal mood swings from the Pill as it has no hormones in it at all).
It delivers a low dose progestogen and is worn for three years. It’s inserted and removed under local anaesthetic by a doctor or family planning nurse.
Pros You can have one put it three weeks after birth and use it while breast-feeding. Could reduce painful, heavy periods. Fertility returns to normal once removed.
Cons Could cause weight gain, breast tenderness, acne and mood changes or irregular bleeding, spotting or periods stopping.
The injection
PROBLEM: ‘I get terrible PMS’
TRY: The injection
The ‘Depo-Provera’ aka the injection, is injected into the buttocks, arm, leg or abdomen every eight to 13 weeks. As it’s progestogen only it suits women who are sensitive to oestrogen and unlike the combined Pill, it’s not affected by other medicines such as those for epilepsy.
Pros You don’t have to think about it for 8-13 weeks. You can use it while you’re breastfeeding. According to the Family Planning Association, it might help reduce heavy, painful periods and help symptoms of premenstrual syndrome.
Cons It may lead to weight gain. According to Dr Connolly, many women will spot for about a year after using the Depo Provera and after that, the majority will find their periods will stop. Fertility can take 10 months to a year to return to normal after you’ve stopped having the Depo-Provera.
If you gain weight easily on contraception – avoid the injection
PROBLEM: ‘The Pill makes me put on weight’
TRY: Any of the LARCS above except the injection
‘There is no evidence that any of the LARCs lead to weight gain, except the Depo-Provera, the injection,’ says Dr Connolly. One in four women will put on weight with it, she says.
If your GP isn’t keen to talk about alternatives to the Pill, look up your local family planning clinic and book in to see them. All types of contraception are covered by the NHS, and you won’t have to pay for any method you choose. You can also download a free app to help you find a contraception clinic.
Relevant Healthista Content:
I tried a new libido booster pill and this is what happened
10 perimenopause symptoms that could explain your moods, aches and low libido
Healthista Content you may also like:
4 hormones that help you lose weight from exercise – Body Transformation Week 10
The new shorts that helped this woman’s urinary incontinence
Menopause: 5 things this TV superstar wants you to know
Tired all the time? You might have sleep apnoea – here’s a doctor’s guide on what to do
Like this article? Sign up to our newsletter to get more articles like this delivered straight to your inbox.