Cara Delevingne, Kim Kardashian and Liam Gallagher all suffer with the debillitating skin condition but now, doctors know more than ever about how to treat it. We talk to Professor Chris Griffiths, a world expert on the condition
If you have psoriasis, know that celebs such as Cara Delevingne, Kim Kardashian and Lee Ann Rimes also have it is probably little consolation if yours isn’t under control. But you don’t have to live with it as there is more than ever that can be done today for psoriasis suffererers, says Christopher Griffiths, Professor of Dermatology at the University of Manchester and a world expert on psoriasis.

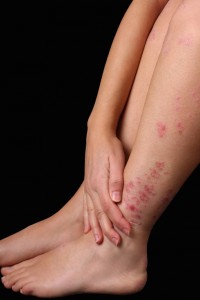
Characterized by raised flaking, itching red patches on various parts of the body, psoriasis affects around 1.8 million people in Britain – most of them before their 40th birthday.
It’s is an immune condition with a strong genetic component, where the body fails to control the level of cell turnover in the skin. Cells accumulate and cluster as red, inflamed patches that can thicken the skin and often have a ‘silvery scale’ appearance.
In most cases psoriasis is genetically pre-determined, but you may never get the triggers that can activate those genes to launch an attack, explains Professor Griffiths.
‘If have a genetic pre-disposition for psoriasis it may appear for the first time after a virus or infection such as streptococcal sore throat or tonsilitus when the immune system is weakened or it can come on after a stressful event,’ says Professor Griffiths.
Indeed, ‘though even after treatment, patients will have the susceptibility to develop psoriasis again, many go into remission for many years between attacks’, he says.
But around 30 percent will also get painful joints (sometimes the joint pain comes before the skin condition appears) as the immune system targets the joints to trigger ‘psoriatic arthritis’.
Treatments for psoriasis
Avoid soap Dermatologists recommend avoiding soap which can dry the skin and make flaking worse, and replace it with emollient washes (such as Dermol Shower Emollient £6.65) and unperfumed moisturisers such as E45.
Coal tar For the last 100 years products containing coal tar, a thick, heavy oil with a strong smell have been used for psoriasis and today, they’re still used as treatments in some centres in conjunction with UVB light therapy, says Professor Griffiths. ‘But they’ve fallen out of favour as a treatment as there are so many newer treatments that work as well and coal tar can be unpleasant and messy for patients to use’, he explains.
Vitamin D ointments Mild cases of psoriasis can be treated by your GP who may prescribe gels used once daily containing vitamin D ointments combined with a corticosteroid which can reduce the turnover of the top layers of the skin. Vitamin D inhibits the active turnover of the top layer of skin and there is some evidence that it can dampen down the immune response that occurs in psoriasis while the corticosteroids have a mild anti-inflammatory effect, explains Professor Griffiths.

Light therapies Though specialists may recommend a course UVA-based light treatment called PUVA. This is where light therapy is combined with Psoralen tablets (taken orally or dissolved in bathwater) which increase the skin’s sensitivity to the light and 85 percent effective. Though available on the NHS its use is not as widespread as it once was because of newer, less dangerous treatments.
‘There is good evidence to show that PUVA causes skin cancer if it’s used in large amounts,’ says Professor Griffiths. ‘When it was introduced 40 years ago, the risks hadn’t been determined and though it was highly effective, people used it too often and it not only increased their sun damage such as wrinkles and brown spots but also their incidence of skin cancer because the treatment increased their skin’s sensitivity to the damaging effects of sunlight to such a degree’. It’s still used and available on the NHS but patients are limited to how many treatments they can have, about one a year – you’ll also have to wear protective sunglasses outside at all times on the day of your treatment as your eyes also become sensitive to light along with your skin.
Instead, specialists now favour narrow band UVB (see eczema) for psoriasis treatment in combination with coal tar treatment. ‘It’s as effective as PUVA treatment for psoriasis and comes with far fewer risks of skin cancer,’ says Professor Griffiths.
Newer treatment options available for psoriasis
‘Biologic’ therapies One new treatment has transformed the lives of patients with severe psoriasis in the last decade, says Professor Griffiths. New ‘biologic’ injections help block the chemicals that lead to the immune response involved in psoriasis, particularly if psoriatic arthritis is a problem.
They’re injected by the patient just under the skin (similar to self-injected insulin for diabetes) from once a week to once every 12 weeks, depending on the type of treatment.
‘We have four biological therapies approved by the National Institute for Clinical Excellence (NICE) for the treatment of psoriasis and over the next year or so at least one more will be approved with even better effectiveness. This means we can treat patients who 30 years ago would have been having significant amounts of PUVA, spending time in hospital and increasing their skin cancer risk. Now they can have normal lives,’ says Professor Griffiths.
However, the drugs are expensive and come with a high risk of side effects including an increased risk of infection, rashes in other areas and in rare cases neurological symptoms.

Apremilast Ground-breakingly, a new once-a-day tablet could become available in the UK in the next year. Called Apremilast, it works by inhibiting an enzyme in immune cells causing an anti-inflammatory effect.
Trials on the drug in the US have been promising and NICE are currently reviewing it as a treatment for UK patients.
Professor Griffiths who has conducted clinical trials using the drug in the UK says: ‘This is a new class of ‘small molecule’ medicine taken orally that target phosphodiesterase 4 (PDE4), an enzyme in immune cells producing an anti-inflammatory effect and so far, the results have been promising. If approved by NICE, it could further revolutionise the treatment of psoriasis.’
Psoriasis Awareness Week runs from November 1st-8th. Find out more at the Psoriasis Association
RELATED:
5 best creams to help psoriasis (PLUS how diet can help)
Like this article? Sign up to our newsletter to get more articles like this delivered straight to your inbox.




















































