British MPs have voted to allow 3-person IVF or ‘mitochondrial transfer’ which means doctors will in the future be able to prevent major childhood diseases by making babies using IVF and genetic material from three people. So what is it?
The three person IVF technique, known as mitochondrial transfer, has been pioneered at Newcastle University and after MPs approved the regulations, it could be available on the NHS this year. Britain will be the first country in the world to offer it.
But what is 3-person IVF and how is it done? Healthista spoke to Dr Geetha Venkat, Director of Harley Street Fertility Clinic to find out
What is mitochondrial transfer or ‘3-person IVF’? Some serious genetic diseases such as muscular dystrophy, heart and liver conditions are passed on through the DNA found in maternal mitochondria. Mitochondria are the energy factories of cells, found in the substance that surrounds the nucleus of a cell called cytoplasm. Most of the genes that make us who we are – about 23,000 – are contained in the nucleus of the cell. There is some genetic material in the mitochondria but very little – only 37 genes. Currently if a woman is a carrier of mitochondrial disase, our only choice is to use donor eggs. In mitochondrial transfer, the faulty mitochondria is replaced by the donor’s healthy one. That way the baby will have all the genetic material of its parents with the diseased genes removed. The mitochondria from the donor will contain some genes from the donor, though the majority will be from the parents.
the baby will have all the genetic material of its parents with the diseased genes removed.
Does it mean the child has three sets of genes – mum, dad and donor? Yes but most of the genetic material will come from the mother and father and only a tiny amount of genetic material will come from the donor.
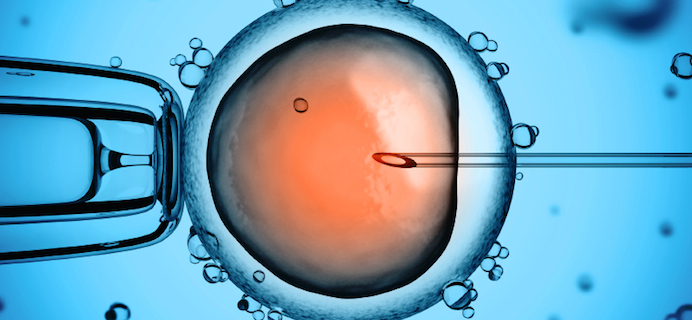
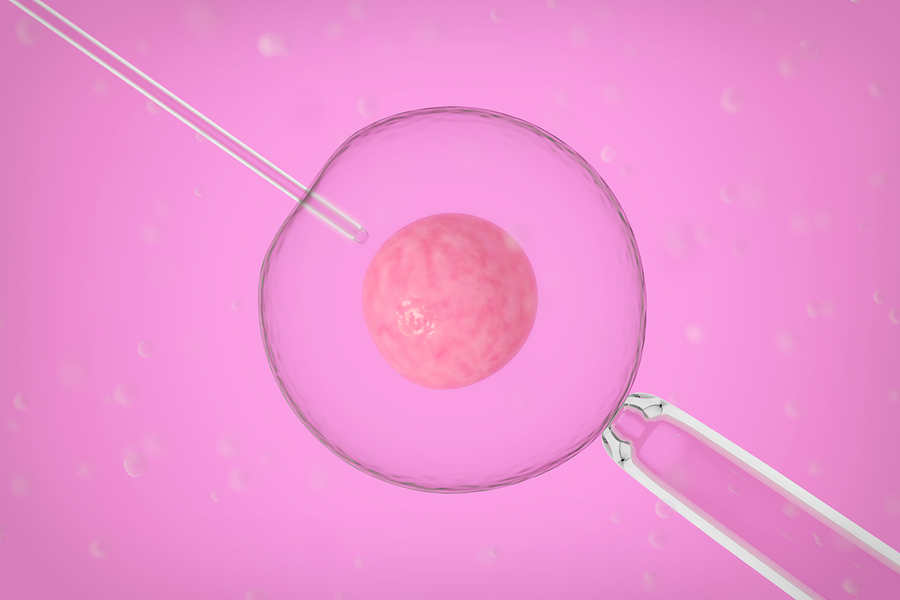
How is it done? The egg is fertilized with sperm using IVF and then, under a microscope using a tiny needle, the nucleus is sucked out of the fertilized egg and put it into the cytoplasm of the donor’s egg (after the nucleus of the donor egg has been removed).
Why are doctors calling it such a breakthrough? Up to now, we could only use donor eggs if there was a mitochondrial disease in the family which meant the child would have no genetic material from its mother. I too think it’s a breakthrough because it means if a woman is carrying a mitochondrial disease she can have her own children without passing on diseased genes, and still pass on her own genes to her child.
Will the mitochondrial donor be recorded as one of the parents? Not on the birth certificate.
Could it be used in fertility treatment as an alternative to donor eggs, say to increase the quality of older eggs? The idea has been trialled in research though it’s not at human stage. Called Cyctoplasmic Transfer, it takes the genetic material from the nucleus of the mother and puts it into the younger donor egg hence increasing its quality and theoretically increasing its chances of being fertilized. This might increase the chances of conceiving in women over 40 who might otherwise only have been able to use donor eggs but trials have not reached human stage yet.
Like this article? Sign up to our newsletter to get more articles like this delivered straight to your inbox.