It’s good for your baby, but not every mother finds breastfeeding comes naturally. Here’s what to do if you’re trying to but can’t breastfeed says world-leading researcher and infant feeding expert Professor Amy Brown
The case in favour of breastfeeding is incredibly positive; it protects against a whole range of illnesses, and reduces your risk of developing heart disease, cancer and diabetes.
Breastfeeding also saves you buying formula and once you’ve got the hang of it, breastfeeding can be rewarding and far quicker and easier than having to make up bottles.
Recently published research has even found a potential connection between the duration a mother breastfeeds and the child’s GCSE scores, but this topic requires a lot of nuance.
Breastfeeding also hit the headlines a few years ago when ultra-marathon runner, Sophie Power, 36, was snapped breastfeeding her three-month-old son mid-race and the photo went viral.
While some detractors questioned whether Power should have run, the response on social media was mainly positive; Power was not in fact allowed to defer her place, so the choice was run or lose the opportunity.
And why wouldn’t it be? It’s hard to think of a better ad for breastfeeding. Power, who had just run 50 miles looks composed, especially compared to the male runner lying next to her flat on his back.
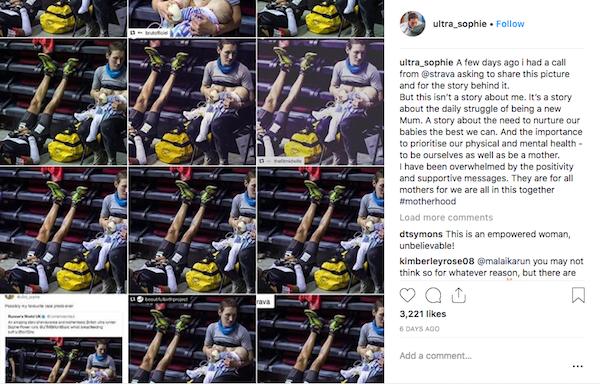
Whether you are runner or not, there’s no doubt that breastfeeding is great for you and your baby. And as we’ve seen from these shots, breastfeeding doesn’t need to get in the way of your life or fitness.
breastfeeding protects against a whole range of illnesses, and reduces your risk of developing heart disease, cancer and diabetes
But that doesn’t mean it always comes easy. Those early weeks can feel really challenging and it’s normal to have all sorts of worries. Is he getting enough milk? Am I latching her on right? Is feeding in public ok?
An infant feeding survey conducted by the NHS found that 80 per cent of women who stop breastfeeding in the first 6 weeks are not ready to do so – and most stop for reasons that with the right support and information could have been prevented. It also found that in the UK, just half of women are breastfeeding by six weeks compared to 90 per cent in Scandinavia.
Knowledge is power, so here are some of the top breastfeeding concerns and what you can do about them. from world-leading researcher and infant feeding expert and author of new book, world-leading researcher and infant feeding expert Professor Amy Brown.
1. It will hurt
It’s common to worry that breastfeeding will hurt, but with the right advice and support, it shouldn’t. The sensation can sometimes take a little getting used to, but any pain that lasts more than a brief few seconds, is excruciating rather than uncomfortable, or damages your nipple needs sorting out. But the good news is that there are plenty of trained professionals out there who can help you.
The key to comfortable feeding is getting your latch right. Lots of people imagine a baby just sucking on the nipple like a straw but when a baby latches on correctly they take a big mouthful of your nipple and surrounding darker skin (your areola) and draw your nipple right back into their mouth.
It can be tricky to get this right at first, but it’s really important to persevere as if the latch is not right your baby can damage your nipple and may not get enough milk. A few tiny adjustments in angle or how you are holding your baby could save your nipples. Ask your midwife to check your latch as many times as you like. Check out this La Leche League guide for more information.
If your baby is still struggling and doesn’t seem to be able to get a deep mouthful of breast, talk to your health professional about getting them assessed for tongue tie. Some baby’s tongues are tethered too tightly in their mouths meaning they struggle to latch. Infections such as thrush or mastitis can cause pain too. If you notice any itching or pain in your nipples, or deep in your breasts, or hot, red areas then contact your health professional as soon as possible. All of these things are fixable and do not have to mean the end of breastfeeding.
READ MORE:
2. ‘I won’t be able to make enough milk’
You might have heard stories that lots of women don’t make enough milk. However, with the right knowledge and support most women should make enough milk for their baby. The secret is to feed your baby responsively. This means feeding them whenever they want to be fed, throughout the day and night. Babies often feed at least every 2 – 3 hours, often more. Sometimes they have short feeds, and sometimes longer – just like as adults we don’t eat and drink in a set pattern.
Your body matches your milk supply to how much milk you or your baby remove. When you feed your baby, your body replaces that milk. If you feed frequently, you make more milk but if you try to feed less often or give a bottle your body thinks less milk is needed, so makes less. Your baby is the best judge of whether they are hungry, not the clock. Ignore anyone who suggests your baby feeds too much or should feed in a routine.
if you feed frequently, you make more milk but if you try to feed less often or give a bottle your body thinks less milk is needed, so makes less
You can check whether your baby is getting enough milk by thinking about what goes in and what comes out. Is your baby feeding at least 8 – 12 times in 24 hours? Can you hear them swallowing? If they’re over a week old do they have at least 6 wet and 2 dirty nappies a day? (babies older than 6 weeks might have dirty nappies less frequently). Do they look alert and hydrated? For more signs check out the Baby Friendly website.
Some health conditions such as diabetes or thyroid disorders mean you might not make enough milk. Sometimes women do not have enough glandular tissue in their breasts (known as hypoplasia) so might make less milk. If you have this you probably noticed your breasts did not change much in pregnancy, may be long and thin, and widely spaced. However, not making a full milk supply does not need to mean the end of breastfeeding – you can still breastfeed alongside formula if necessary. Talk to your health professional about the best ways of making as much milk as possible.
3. ‘I need to take a medication’
It’s natural to worry about taking a medication when breastfeeding but the good news is that in many cases the medication, or an alternative, will be fine. For many medications only a small amount (or sometimes none at all) will pass into your milk which and is not harmful for your baby. There are exceptions including lithium, some arthritis medications and chemotherapy. But talk to your health professional about your options.
If you have been prescribed a medication and are unsure it is safe, or have been told that you can’t breastfeed and take it, you can contact the Breastfeeding Network’s drugs in breast milk service. Led by a pharmacist with many years experience in supporting breastfeeding, they can give you up to date information about different medications.
4. ‘My baby will be less settled’
Lots of people might tell you that formula will make your baby more settled but this isn’t true. Babies having lots of needs is normal. When they were still inside you they had a constant supply of food, warmth and comfort – being born can be quite a shock! Babies are vulnerable and are programmed to want to be held and stay close to you.
Crying is their only way to communicate. They have tiny tummies so need to feed frequently and shorter sleep cycles so wake often. If they do wake at night, they often need help getting back to sleep. Lots of adults wake at night but can tuck themselves back in or get themselves a drink.
These things are just your baby’s way of feeling secure and having their needs met rather than something to be fixed. However often we’re not prepared for this. Our first baby may be the first baby we have spent much time around, or even held. Adverts tell us that babies are smiley, happy creatures. No one tells us how much input new babies need. So we often worry that something is wrong, or needs fixing.
Some people might tell you that formula will solve all of this for you. It won’t. There is no reason why a bottle of formula would change what is normal baby behaviour. Your baby just wants you however they are fed. This can be really tough though, so make sure everyone around you helps by looking after you. After all, you just grew a whole new human, and are now keeping it alive with your boobs – you deserve it!
5. ‘I won’t be able to feed in public’
It can be nerve wracking the first few times you feed a baby in public, sat in an unfamiliar chair, all the while silently thinking ‘I’ve got my breast out in public’. But the number one thing to remember is that you are protected to breastfeed your baby by law wherever and whenever you want. No one can ask you to stop, to move elsewhere, or to leave.
If you are worried you can practice in front of a mirror: strategically drape a muslin cloth, or face away from others – but only do that if it helps you feel more comfortable, not for anyone else. Taking a friend or partner the first few times can help you feel supported too.
But once you’ve got that baby latched on and look up, you’ll most likely find that no one has noticed. Although we might hear stories where women have been harassed or asked to feed in a toilet, many thousands of women breastfeed their babies every day without issue. You might even find, like I did, that people come up and talk to you, or even stoke your baby’s head, without even realising they are feeding!
6. ‘My partner won’t bond with the baby’
This one is so common to hear but absolutely does not need to be true. There are so many ways to bond with a baby; giving them a bath, cuddling them in a sling, or taking them out for a walk in between feeds. Your partner could sit with, so you’re all cuddled up together. And when they’re a little older (it’s best to wait for around 6 weeks to get your supply sorted) if you’re both happy, you can express a feed for them to give. Some couples choose the feed before bed so you can get a head start on some sleep.
It’s also important to remember that although we might have an idyllic image of giving a baby a bottle, it doesn’t always work out that way. Some babies refuse a bottle. And then there’s the sterilising and preparing and buying of formula. There can be more relaxing ways to bond!
7. ‘My diet isn’t healthy enough’
Eating healthily is important, but that’s mainly to make sure you feel as strong as possible. The human body is clever, and will prioritise making sure your baby gets enough milk, but if your diet is not great, then it’s you who might end up feeling a bit rubbish. But you don’t have to worry about your milk – what you eat doesn’t really have any impact on its nutrients. Focus on good foods that nourish and help repair your body after birth – but there’s no need to be really strict. Cake definitely has its place.
Hopefully you are now feeling more confident about breastfeeding your baby. If you have any further questions, you can contact the National Breastfeeding Helpline, open 9.30am – 9.30pm 365 days a year (0300 100 0212). Calls are answered by trained experts, who have breastfed their own babies. For extra support and friendly faces, ask your health professional for details of your local breastfeeding peer support group. Breastfeeding mums and trained supporters can help answer your queries or just sympathise about your shared exhaustion, often over cake.
The Positive Breastfeeding Book: Everything you need to feed your baby with confidence by Amy Brown is published by Pinter & Martin £14.99

With a background in psychology, she first became interested in the many barriers women face when breastfeeding after having her first baby.
Three babies and a PhD later she has spent the last twelve years exploring psychological, cultural and societal barriers to breastfeeding, with an emphasis on understanding how we can better support women to breastfeed and subsequently raise breastfeeding rates.
Find out more: breastfeedinguncovered.co.uk Follow Professor Brown on Twitter: @Prof_AmyBrown
Like this article? Sign up to our newsletter to get more articles like this delivered straight to your inbox.























































